Car accidents leave more than physical scars. Most people don’t realize that the emotional aftermath-anxiety, nightmares, and depression-can be just as debilitating as broken bones or whiplash.
At Schaar & Silva LLP, we’ve seen firsthand how accident victims struggle with the psychological weight of their injuries. That’s why emotional support in Santa Cruz is so important during recovery.
This guide walks you through how counseling actually helps, where to find affordable mental health services locally, and how to build a recovery plan that addresses both your body and mind.
What Happens to Your Mind After a Car Crash
The moment a car hits you, your nervous system floods with adrenaline and cortisol within seconds. Your body shifts into survival mode, triggering reactions like shakiness, rapid heartbeat, or an eerie sense of calm that feels disconnected from reality. In the first week after a crash, about 46 percent of survivors experience panic attacks, according to the American Psychological Association. These aren’t minor stress responses-they’re your brain protecting itself from overwhelming input through emotional numbness or dissociation.
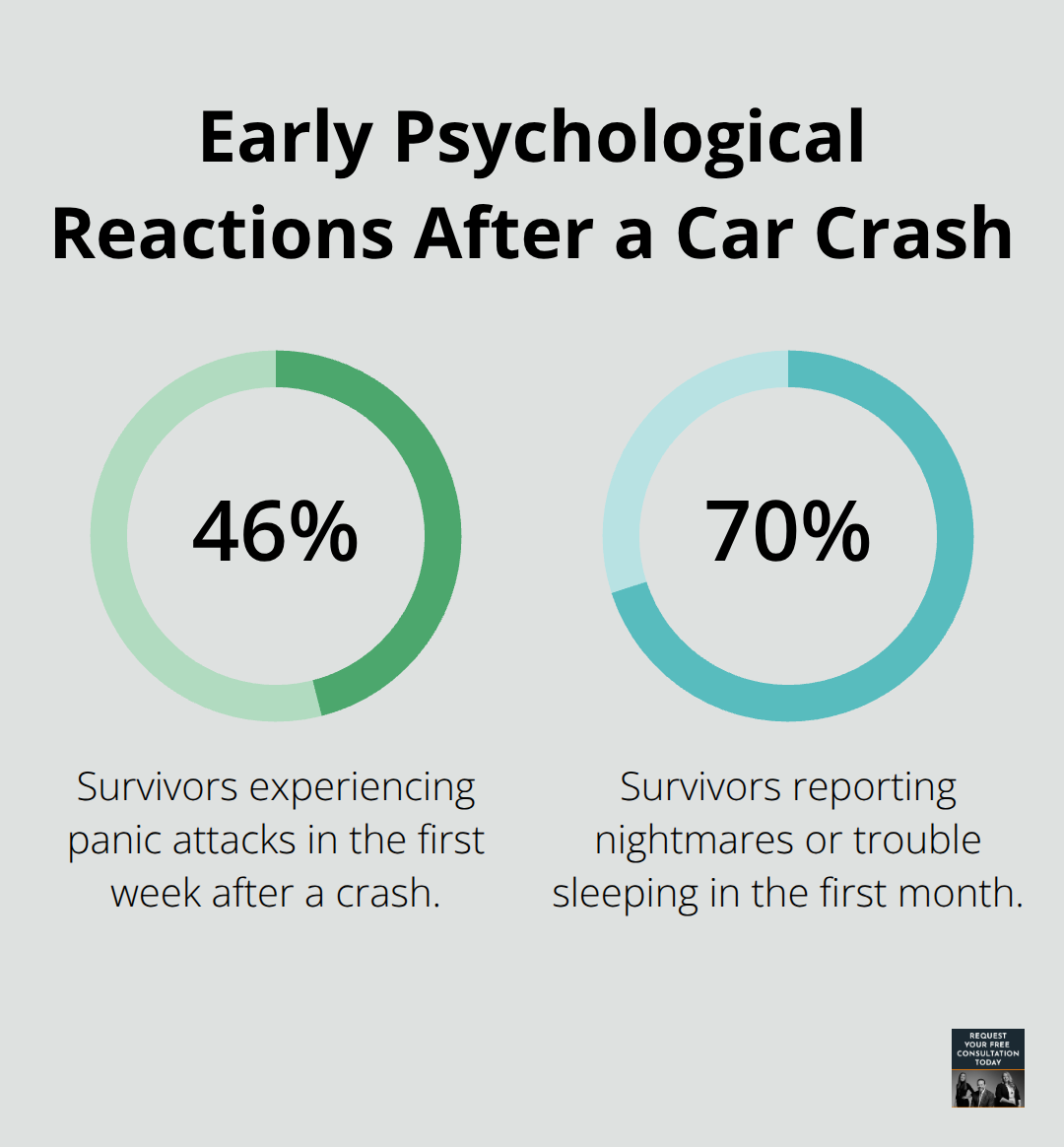
Sleep disruption follows quickly, with up to 70 percent reporting nightmares or trouble sleeping in the first month. These reactions are normal, not signs of weakness.
The Long-Term Mental Health Toll
Within six months, the statistics become harder to ignore. Roughly 39.2 percent of survivors develop anxiety disorders, 17.4 percent develop depression, and 32.3 percent develop PTSD, according to the Journal of Clinical Medicine. Women face about 2.5 times higher risk of PTSD than men. If you had anxiety or depression before the crash, the accident typically amplifies those conditions, making early intervention critical. Avoidance behaviors emerge in about 39.2 percent of survivors within six months-steering clear of certain routes, highways, or driving altogether. Depression affects roughly 70 percent of those with depressive symptoms through concentration problems, making work and daily tasks feel impossible. In Santa Cruz County, where 54 percent of adults aged 18-24 have seriously thought about suicide, the mental health crisis hits young accident survivors particularly hard.
How Physical Pain Intensifies Emotional Damage
Here’s what most people miss: persistent physical pain six to eight weeks after the crash strongly predicts greater depression severity about two months later. Your body and mind aren’t separate systems. Chronic pain activates the same neural pathways as emotional trauma, meaning a broken leg or spinal injury doesn’t just cause physical suffering-it compounds your psychological distress. This interaction hinders rehabilitation progress, weakens immune function, and slows overall recovery. The brain-body link means that addressing only your physical injuries while ignoring emotional trauma leaves you stuck in a cycle of pain and depression that feeds itself.
Why Professional Help Matters Now
The interaction between physical recovery and mental health creates a critical window. Early, evidence-based therapy yields strong results: cognitive-behavioral therapy with gradual exposure can yield about 85 percent improvement for travel-related fears in 12–16 sessions, while EMDR can reduce PTSD symptoms by about 77 percent in 6–12 sessions. These aren’t theoretical outcomes-they’re documented results from peer-reviewed trauma treatment literature.
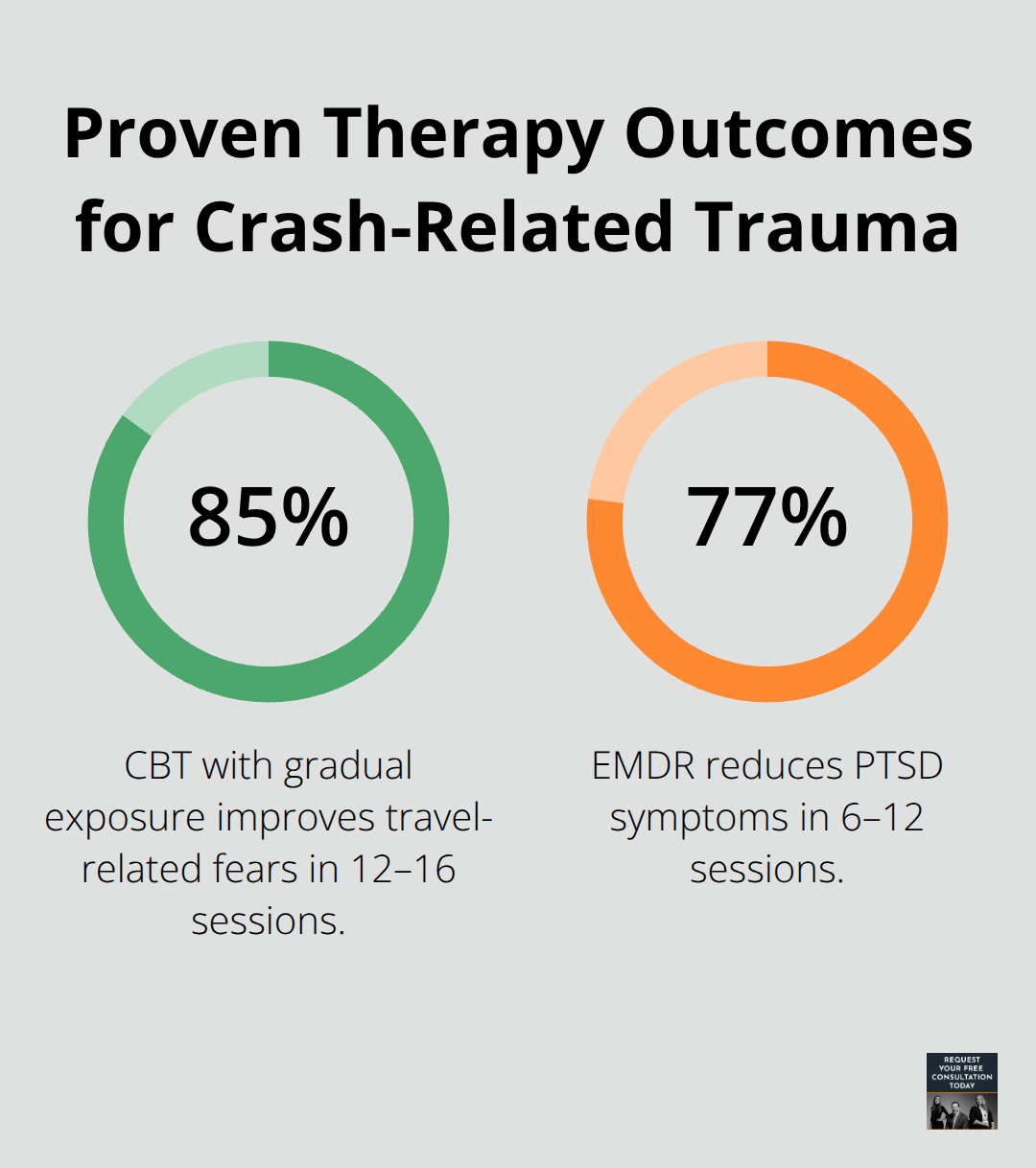
Waiting six months or longer to address emotional symptoms makes recovery significantly harder. The sooner you connect with a counselor who understands accident-related trauma, the faster you can interrupt the pain-depression cycle and move toward actual healing.
How Counseling Rewires Your Response to Trauma
Structured therapy doesn’t just let you talk about what happened-it rewires how your brain processes the accident. Cognitive-behavioral therapy works by breaking the connection between the crash memory and your current fear response. Instead of your mind treating every car ride as a repeat of the accident, CBT gradually reintroduces safe driving situations while teaching you to recognize and challenge catastrophic thoughts. According to peer-reviewed trauma treatment literature, CBT with gradual exposure delivers about 85 percent improvement for travel-related fears in 12 to 16 sessions. EMDR therapy takes a different approach, using guided eye movements to help your brain reprocess the traumatic memory so it loses its emotional charge-research shows EMDR reduces PTSD symptoms by about 77 percent in 6 to 12 sessions. The key difference from casual support is that these methods target the specific neural pathways activated during your crash, not just your general stress levels.
Finding a Trauma-Informed Counselor in Santa Cruz County
A trauma-informed counselor in Santa Cruz County will assess which approach fits your situation. You’ll find more than 500 trauma and PTSD counselors listed on Psychology Today, where you can filter by credentials like LMFT, PsyD, PhD, or LCSW and check which ones accept your insurance. Most major insurers operate in Santa Cruz County and cover trauma-focused therapy-Aetna, Cigna, Anthem, UnitedHealthcare, Blue Shield, and Medi-Cal all participate-often with sliding-scale fees if cost creates a barrier. Start by telling your therapist immediately that you were in an auto crash so their notes capture the exact onset of symptoms and how the accident affects your daily functioning.
Physical Movement Rebuilds Emotional Resilience
Coping strategies after an accident extend far beyond the therapy office. The Virtual Wellness Experience, hosted by the Santa Cruz County Office of Education, offers bite-sized mindfulness, yoga, and dance videos designed for quick coping during recovery-these aren’t lengthy commitments but tools you can use on difficult days when anxiety spikes or nightmares disrupt sleep. Physical exercise acts as a documented protective factor for mental health in Santa Cruz County, directly counteracting the depression and concentration problems that plague 70 percent of accident survivors with depressive symptoms. Walking, swimming, or gentle strength training doesn’t just distract you-it reduces cortisol levels and rebuilds the sense of control your body lost during the crash. Pair this with consistent sleep habits, which directly combat the nightmares and insomnia affecting 70 percent of survivors in the first month.
Social Connection Interrupts the Isolation Cycle
Isolation amplifies trauma, but participation in support groups-whether through Mothers Against Drunk Driving, the Trauma Survivors Network, or the Crash Support Network-connects you with people who understand the specific weight of accident-related fear. These groups provide structured coping strategies, not just sympathy. When you coordinate your recovery plan with Schaar & Silva LLP, we connect you with counselors experienced in accident trauma while handling medical lien services so therapy costs don’t drain your resources during healing. The next step involves understanding how to document your emotional recovery in ways that support both your healing and your legal claim.
Where to Find Mental Health Support in Santa Cruz County
Santa Cruz County has 914 mental health providers per 100,000 people according to local mental health data, which means access to qualified counselors is genuinely available if you know where to look. Psychology Today lists more than 500 trauma and PTSD counselors in the area, and you can filter immediately by credentials like LMFT, PsyD, PhD, or LCSW to narrow your search to providers with formal training in accident-related trauma. The critical step most accident survivors skip is telling your counselor during the first appointment that you were in a car crash, not just mentioning it casually. This ensures their clinical notes capture the exact onset of your symptoms and document how the accident affects your concentration, sleep, and daily functioning, which becomes essential if you later need to support a legal claim. Major insurers operating in Santa Cruz County-including Aetna, Cigna, Anthem, UnitedHealthcare, Blue Shield, and Medi-Cal-all cover trauma-focused therapy, often with sliding-scale fees available if cost creates a barrier to getting started immediately.
Choosing Between Different Therapy Approaches
Your first session should involve the counselor recommending either CBT with gradual exposure, EMDR, or Cognitive Processing Therapy based on your specific symptoms and crash circumstances. If a provider doesn’t explicitly discuss which evidence-based method they’ll use, that’s a red flag worth addressing directly. Hospital-backed groups like Kaiser Permanente offer trauma and grief programs within their network, while UC Davis Hospice runs six-week sessions focused on trauma recovery if you prefer a structured timeline. The 988 Suicide and Crisis Lifeline operates 24/7 if you experience suicidal thoughts or overwhelming panic between therapy sessions, providing confidential support without judgment. Start documenting your emotional recovery from day one: note panic attacks, sleep disruption, avoidance behaviors, and concentration problems in a symptom diary, and share these observations with your counselor so treatment records reflect the severity and timeline of your trauma.

Coordinating Mental Health Care with Your Legal Recovery
When you work with Schaar & Silva LLP, we connect you with counselors experienced in accident trauma while handling medical lien services so therapy costs don’t drain your resources during healing. This coordination matters because your therapy records, paired with documentation of physical injuries and lost work time due to anxiety or depression, strengthen insurance and court claims significantly. Your counselor’s credentials and consistent treatment notes create objective evidence of emotional harm that insurance companies cannot dismiss as exaggeration. Collecting medical records from your initial ER visit, including vital signs and observations about your emotional state, establishes that trauma started immediately after the crash rather than weeks later, which carriers often dispute. Therapy costs, prescribed medications for anxiety or depression, and documented lost wages become legitimate damages when supported by qualified mental health records, turning your recovery plan into both a healing tool and a documented claim.
Final Thoughts
Your recovery after an auto accident isn’t linear, and it doesn’t happen in isolation. The most successful healing paths combine three elements: professional mental health treatment, coordinated legal support, and active participation in your own recovery decisions. Start your recovery plan immediately after the crash, not months later when avoidance behaviors have solidified and depression deepens.
Santa Cruz County offers genuine resources for accident survivors, with 914 mental health providers per 100,000 people making qualified counselors accessible. Support networks like MADD, the Trauma Survivors Network, and the Crash Support Network connect you with people who understand the specific weight of accident-related trauma. Use the Virtual Wellness Experience for daily coping tools, incorporate physical movement into your routine, and prioritize sleep as aggressively as you would physical therapy.
When you work with Schaar & Silva LLP, we handle the legal complexity while you focus on healing and emotional support in Santa Cruz. We connect you with counselors experienced in accident trauma, manage medical lien services so therapy costs don’t drain your resources, and ensure your emotional recovery is documented in ways that support both your healing and your claim. Taking control of your recovery means refusing to separate your emotional healing from your legal recovery, refusing to wait for symptoms to worsen before seeking help, and refusing to let isolation compound your trauma.

