A car crash leaves more than physical marks. The emotional trauma that follows can be just as debilitating as broken bones or whiplash, affecting your sleep, relationships, and daily life.
Many accident survivors don’t realize that psychological healing requires the same attention as physical recovery. At Schaar & Silva LLP, we understand this reality and help clients access the mental health resources they need to move forward.
Why Your Mind Needs the Same Care as Your Body
A car crash activates your fight-or-flight response, flooding your body with stress hormones like cortisol and adrenaline. Once the immediate danger passes, your nervous system should return to baseline-but for many accident survivors, it doesn’t.
The Timeline of Psychological Injury
Within one month after a crash, roughly 29.4% of survivors meet the clinical threshold for post-traumatic stress disorder according to research in peer-reviewed trauma literature. Three months later, that figure drops to 18.8%, but without intervention, symptoms persist for years.
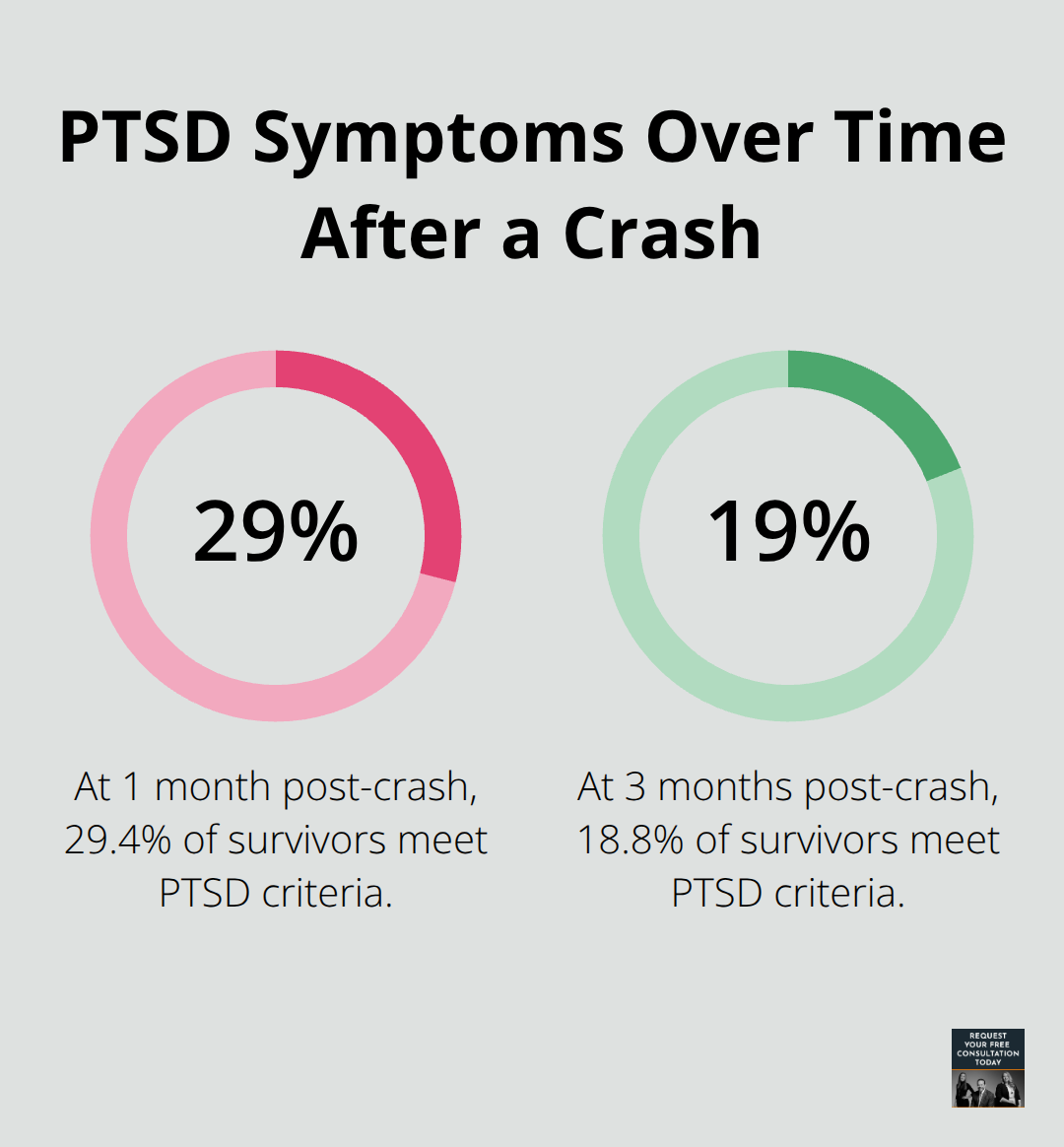
Physical injuries heal on their own timeline, but psychological trauma requires active treatment. Women face approximately 2.5 times higher risk of developing PTSD than men after a crash, and those hospitalized for injuries show significantly higher PTSD rates than those treated in emergency departments.
The Journal of Clinical Medicine reports that within six months post-crash, about 39.2% develop anxiety disorders, 17.4% experience depression, and 32.3% meet PTSD criteria. Sleep disruption hits hard-up to 70% of survivors report nightmares or insomnia in the first month, while 46% experience panic attacks in the first week. These aren’t signs of weakness; they’re normal neurological responses to trauma that respond well to evidence-based treatment.
How Your Brain Processes the Crash
Your brain categorizes the crash as a threat your body couldn’t escape, and it stores the memory differently than normal experiences. This explains why certain triggers (a similar car sound, a particular road, or even a smell) can cause intrusive thoughts, flashbacks, or physical panic responses without warning. Depression compounds this effect by affecting concentration and motivation, making it difficult to work, drive, or manage daily tasks. The longer these symptoms go untreated, the more entrenched they become in your nervous system.
Evidence-Based Treatments That Work
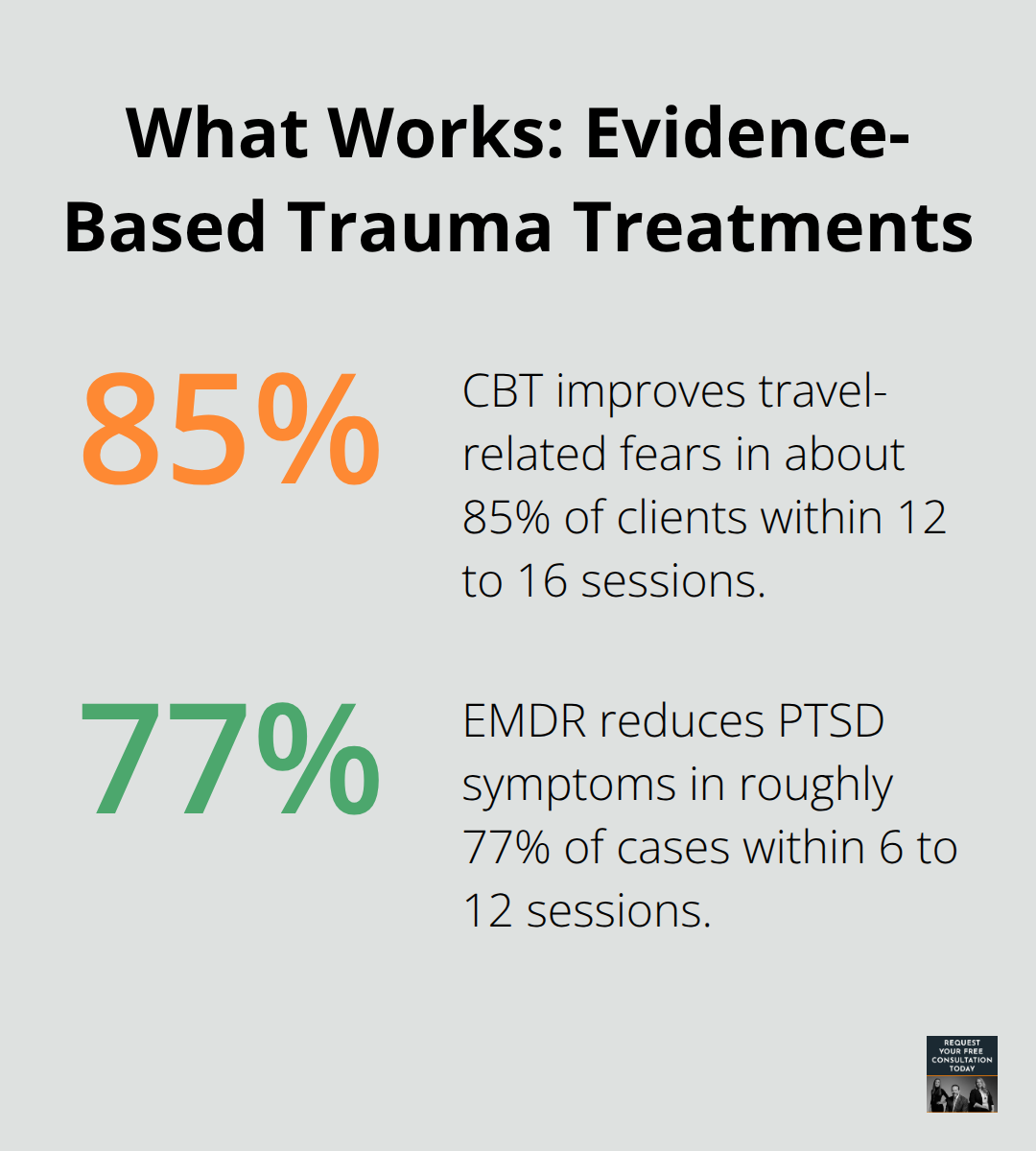
Cognitive behavioral therapy works by rewiring these threat associations, with about 85% of clients showing improvement in travel-related fears over 12–16 sessions. EMDR therapy reduces PTSD symptoms in approximately 77% of cases within 6–12 sessions through reprocessing the traumatic memory itself. These treatments address the root cause rather than just masking symptoms, allowing your brain to integrate the experience and move forward.
Schaar & Silva LLP connects you with mental health professionals who understand crash trauma specifically, and we coordinate medical lien services so therapy costs don’t drain your resources while your case resolves. The next section covers the immediate coping strategies you can start using today, even before you connect with a therapist.
Immediate Coping Strategies You Can Use
Interrupt Panic With Grounding Techniques
The first week after a crash floods your body with stress hormones and keeps your nervous system in high alert. Panic attacks strike 46% of survivors in that initial seven-day window according to the American Psychological Association, so your racing heart and shallow breathing are normal responses, not signs of weakness. Grounding techniques interrupt this panic response by anchoring you to the present moment instead of the crash memory. The 5-4-3-2-1 technique works by naming five things you see, four you can touch, three you hear, two you smell, and one you taste-this sensory inventory forces your brain to process your current environment rather than the trauma.
Use Your Breath and Body to Calm Your Nervous System
Deep breathing activates your parasympathetic nervous system, the part that calms you down. Inhale for four counts, hold for four, exhale for six-the longer exhale matters most. Practice this for five minutes when anxiety rises, not just during panic attacks.

Physical movement also reduces cortisol levels; walking for 20 minutes, swimming, or gentle yoga shifts your body out of threat mode. Many survivors find that moving their body in ways that feel safe helps their nervous system recognize the crash is over.
Build Your Support Network Immediately
Your support network becomes your lifeline in the weeks after impact. Talk openly about what happened with trusted friends or family members; emotional suppression actually strengthens PTSD symptoms over time. If isolation feels safer, consider joining a structured group like the Trauma Survivors Network or Crash Support Network where others understand the specific weight of what you’ve experienced. Document everything from day one-keep a symptom diary noting when panic attacks occur, how sleep disrupts, and what triggers flashbacks. This record serves both your healing and any legal claim, showing the real timeline of your psychological recovery.
Schedule Mental Health Screening Within the First Month
Within the first month, schedule a mental health screening; 29.4% of survivors meet PTSD criteria at this point, and early intervention prevents symptoms from calcifying into your nervous system. In Santa Cruz County, Sacramento, and Oakland, you can find 500+ trauma counselors on Psychology Today (filter by credentials like LMFT, PsyD, PhD, or LCSW and check insurance acceptance). Major insurers including Aetna, Cigna, Anthem, UnitedHealthcare, Blue Shield, and Medi-Cal commonly cover trauma-focused therapy, often with sliding-scale fees. At your first appointment, tell your therapist you were in a car crash so notes capture the exact onset of symptoms. If you need immediate support between therapy sessions, the 988 Suicide & Crisis Lifeline operates 24/7 for confidential help.
Schaar & Silva LLP connects you with mental health professionals who understand crash trauma specifically and coordinates medical lien services so therapy costs don’t drain your resources while your case resolves. The next section covers the professional resources and treatment options available in your area, including therapy approaches that address the root cause of your symptoms rather than just masking them.
Finding the Right Mental Health Care After Your Crash
Access Trauma-Focused Therapy in Your Region
Trauma-focused therapy in Santa Cruz County, Sacramento, and Oakland addresses crash-specific symptoms with proven effectiveness, but finding the right therapist matters more than finding any therapist. The Journal of Clinical Medicine shows that within six months post-crash, 39.2% of survivors develop anxiety disorders and 32.3% meet PTSD criteria, yet many never access treatment because they don’t know where to start. Psychology Today lists over 500 trauma counselors across your region filtered by credentials like LMFT, PsyD, PhD, or LCSW, and you can immediately check which ones accept your insurance. Major carriers including Aetna, Cigna, Anthem, UnitedHealthcare, Blue Shield, and Medi-Cal cover trauma-focused therapy with sliding-scale fees available.
Choose Evidence-Based Treatment Approaches
Cognitive behavioral therapy delivers approximately 85% improvement in travel-related fears within 12 to 16 sessions, while EMDR reduces PTSD symptoms in roughly 77% of cases within 6 to 12 sessions according to peer-reviewed trauma treatment literature. When you call to schedule, specify that you need a therapist experienced with car crash trauma so your intake notes capture the exact onset of your symptoms.
This documentation strengthens both your healing trajectory and any legal claim by establishing a clear psychological timeline.
Combine Medication With Behavioral Treatment
Medication plays a supporting role rather than a primary solution for crash-related trauma. Psychiatrists in your area can prescribe SSRIs or other medications to manage anxiety and depression symptoms while you engage in therapy, but medication alone without behavioral treatment shows limited long-term effectiveness. The Santa Cruz County Office of Education’s Virtual Wellness Experience offers free bite-sized coping tools including mindfulness, yoga, and movement videos between therapy sessions.
Connect With Community Support Programs
Community programs like MACRO in Oakland provide civilian crisis response teams trained in trauma-informed care and de-escalation; you can reach MACRO through their intake form or direct line at 510-446-MACRO for non-emergency behavioral health support. Structured support groups through the Trauma Survivors Network and Crash Support Network connect you with others navigating the same psychological recovery, providing accountability and understanding that friends without crash experience often cannot offer. The 988 Suicide & Crisis Lifeline operates 24/7 for confidential support when symptoms spike between appointments.
Coordinate Your Recovery Plan
Recovery requires combining evidence-based therapy, community connection, and consistent self-care rather than waiting for symptoms to fade on their own. At Schaar & Silva LLP, we connect you with mental health professionals who understand crash trauma and coordinate medical lien services so therapy costs don’t deplete your resources while your case resolves.
Moving Forward
Rebuilding your life after an emotional trauma crash happens gradually, not overnight. Start small by sitting in a parked car, then take short drives on familiar routes during daylight hours with someone you trust, allowing your nervous system to recognize these situations are safe now. Your therapist can guide exposure-based exercises that help your brain integrate the experience rather than remain stuck in threat mode.
A long-term wellness plan anchors your recovery beyond the first few months when symptoms typically peak. Continue therapy sessions even after acute panic subsides, because PTSD symptoms can resurface during stressful periods if the underlying trauma remains unprocessed, and physical activity remains non-negotiable-regular walking, swimming, or strength training keeps cortisol levels manageable while supporting the neurological changes that therapy creates. Document your progress in a journal, noting when triggers feel less intense and when you drive without overwhelming anxiety.
We at Schaar & Silva LLP recognize that emotional recovery and legal resolution work together, and we connect you with mental health professionals who understand crash trauma specifically while coordinating medical lien services so therapy costs don’t deplete your resources. Contact us to discuss your complete recovery in Santa Cruz County and beyond.

